Dashboard
Welcome back, Dr. Bao Yuntong • March 29, 2026
Powered by Medical Large Model v3.2 • Diagnostic Accuracy 98.5%
Total Patients
156
↑ 12% increase from last monthPending Cases
24
Please process in a timely manner ⏳AI Diagnostic Accuracy
98.5%
FDA Certified Standard ✅High-Risk Cases
8
Requires specialist review 🔴Welcome to Salus AI Intelligent Ultrasound-Assisted Diagnosis System
👨⚕️ Physician: Brittany Bao
📌 System Features: AI Ultrasound Image Analysis, Gastric/Pancreatic Lesion Diagnosis Assistance, Patient Records Management, Diagnostic Report Generation
⚠️ Important Notice: AI analysis results are for clinical reference only, final diagnosis must be confirmed by licensed physicians
Recent Patient Examination Records
| Patient ID | Patient Name | Age | Gender | Examination Type | Risk Level | Status | Action |
|---|---|---|---|---|---|---|---|
| #178 | James Anderson | 42 | Male | Gastric Ultrasound (Gastric Filling Contrast) | High Risk | Pending | View |
| #076 | Emma Wilson | 35 | Female | Pancreatic Ultrasound (Pancreatic Parenchyma Evaluation) | Medium Risk | Completed | View |
| #103 | Sofia Martinez | 28 | Female | Combined Gastric + Pancreatic Ultrasound | Normal | Completed | View |
| #045 | Michael Brown | 52 | Male | Pancreatic Contrast-Enhanced Ultrasound | Medium Risk | Pending Review | View |
System Workflow
Salus AI Complete Workflow for Gastric/Pancreatic Ultrasound Diagnosis

Gastric/Pancreatic Ultrasound Case Examples

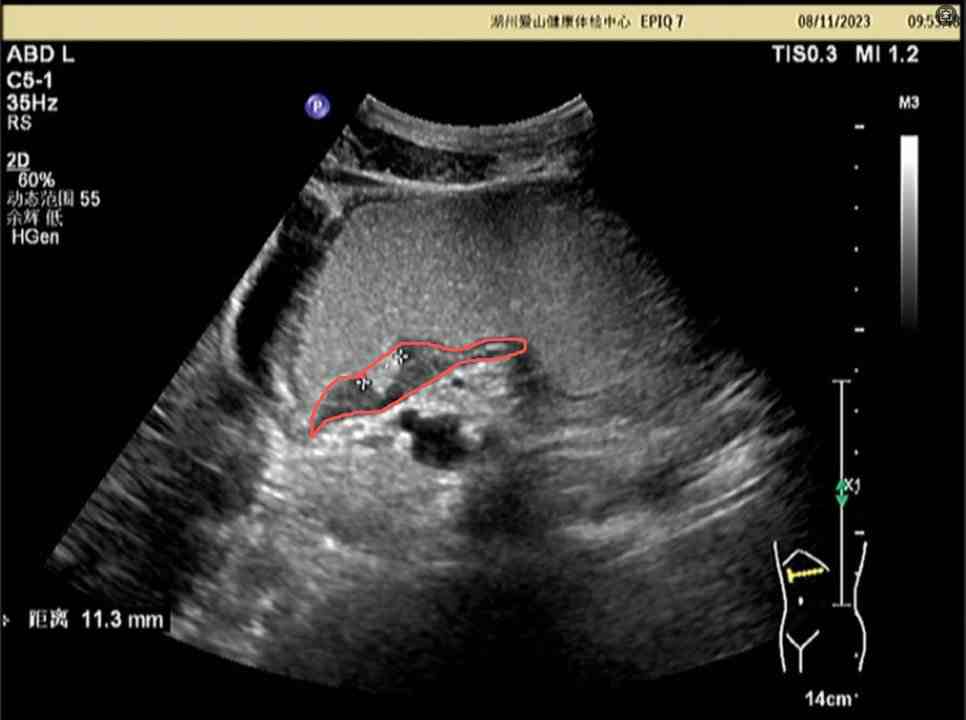
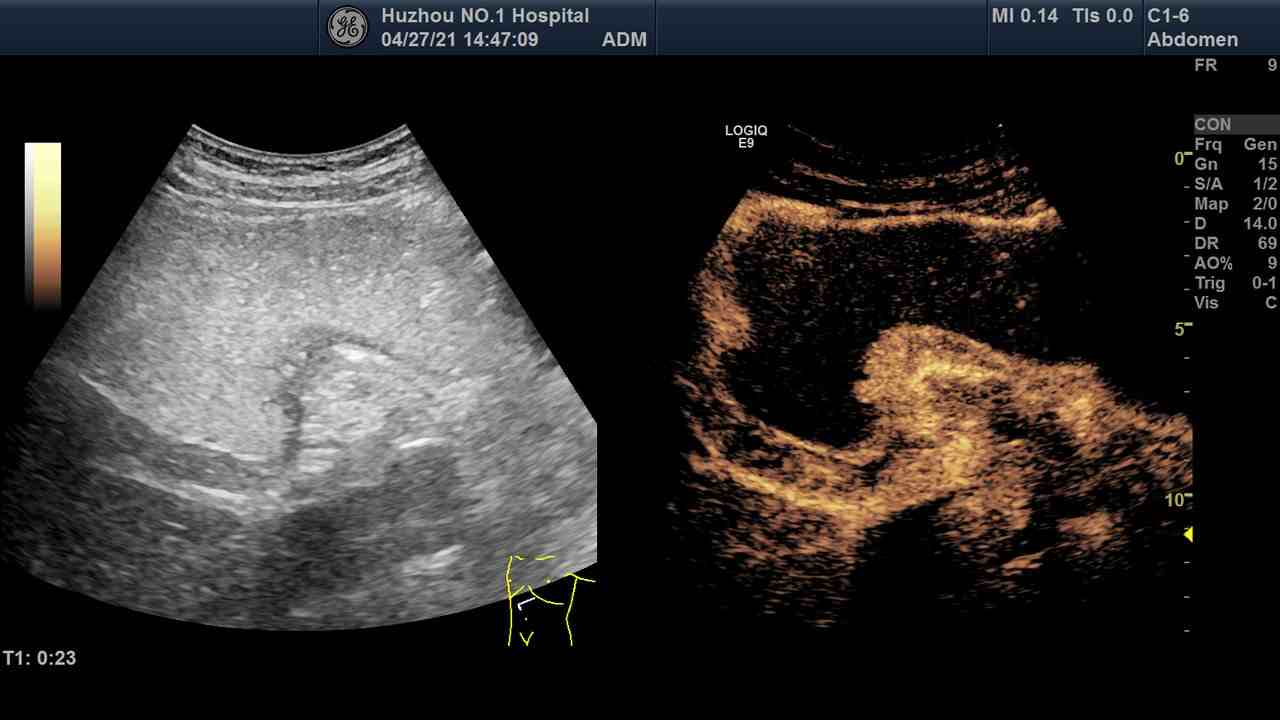
Gastric/Pancreatic Ultrasound Image Upload & AI Analysis
Patient Information & Image Upload
Click or drag to upload gastric/pancreatic ultrasound image/video
AI Diagnostic Analysis Results
Upload gastric/pancreatic ultrasound image and click analyze to view AI diagnostic results
Patient Records Management
All Patient Examination Records
| Patient ID | Patient Name | Age | Gender | Examination Type | Risk Level | Status | Action |
|---|---|---|---|---|---|---|---|
| No medical records available. Please upload gastric/pancreatic ultrasound images to generate medical records. | |||||||
Standard Ultrasound Diagnostic Workflow for Gastric/Pancreatic
AI-Assisted Complete Workflow for Gastric/Pancreatic Ultrasound Diagnosis

2. The AI system can quickly identify lesions such as gastritis, gastric ulcers, pancreatitis, pancreatic masses, with automatic marking of high-risk cases
3. All AI analysis results must be finally reviewed and confirmed by licensed physicians
4. Diagnostic reports are automatically filed and support one-click export, printing, and sharing
